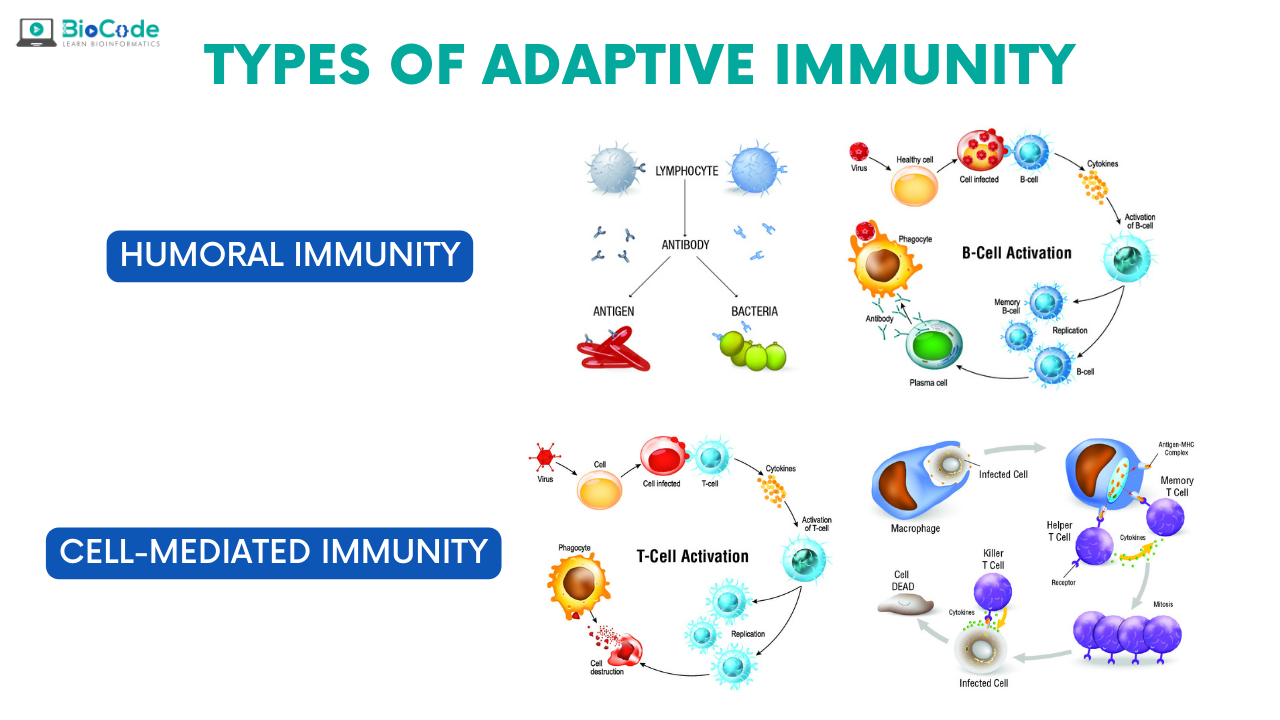
Adaptive Immunity:
The adaptive immune system consists of lymphocytes and their products, such as antibodies. Adaptive immunity develops more slowly and provides more specialized defense against infections. Adaptive immunity, also called specific immunity or acquired immunity. It requires expansion and differentiation of lymphocytes in response to microbes before it can provide effective defense. The adaptive immune system consists of lymphocytes and their products, such as antibodies. Effective for infectious microbes that are pathogenic for humans and may have evolved to resist innate immunity.
Humoral Immunity:
It is mediated by proteins called antibodies, which are produced by cells called B lymphocytes. Secreted antibodies enter the circulation and mucosal fluids, and they neutralize and eliminate microbes and microbial toxins that are present outside host cells, in the body. One of the most important functions of antibodies is to stop microbes that are present at mucosal surfaces and in the blood from gaining access to and colonizing host cells and connective tissues. Antibodies prevent infections from ever being established. Antibodies cannot gain access to microbes that live and divide inside infected cells.
Cell-mediated Immunity:
Defense against intracellular microbes is called cell-mediated immunity because it is mediated by cells, which are called T lymphocytes. Some T lymphocytes activate phagocytes to destroy microbes that have been ingested by the phagocytes into intracellular vesicles. T lymphocytes also kill any type of host cells that are harboring infectious microbes in the cytoplasm. Most T cells recognize only protein antigens, whereas B cells and antibodies can recognize many different types of molecules, including proteins, carbohydrates, nucleic acids, and lipids.
Active Immunity and Passive Immunity:
ACTIVE IMMUNITY
Active immunity may be induced in an individual by infection or vaccination.
PASSIVE IMMUNITY
Passive immunity achieved by an individual by transfer of antibodies or lymphocytes from an actively immunized individual.
Active Immunity
In active immunity, an individual exposed to the antigens of a microbe mounts an active response to eradicate the infection and develops resistance to later infection by that microbe. Such an individual is said to be immune to that microbe, in contrast with a naive individual who not previously exposed to that microbe’s antigens.
Passive Immunity:
In passive immunity, a naive individual receives antibodies or cells (e.g., lymphocytes, feasible only in animal experiments) from another individual already immune to an infection. The recipient acquires the ability to combat the infection for as long as the transferred antibodies or cells last. Passive immunity is therefore useful for rapidly conferring immunity even before the individual can mount an active response, but it does not induce long-lived resistance to the infection. The only physiologic example of passive immunity is seen in newborns, whose immune systems are not mature enough to respond to many pathogens but who are protected against infections by acquiring antibodies from their mothers through the placenta and breast milk.