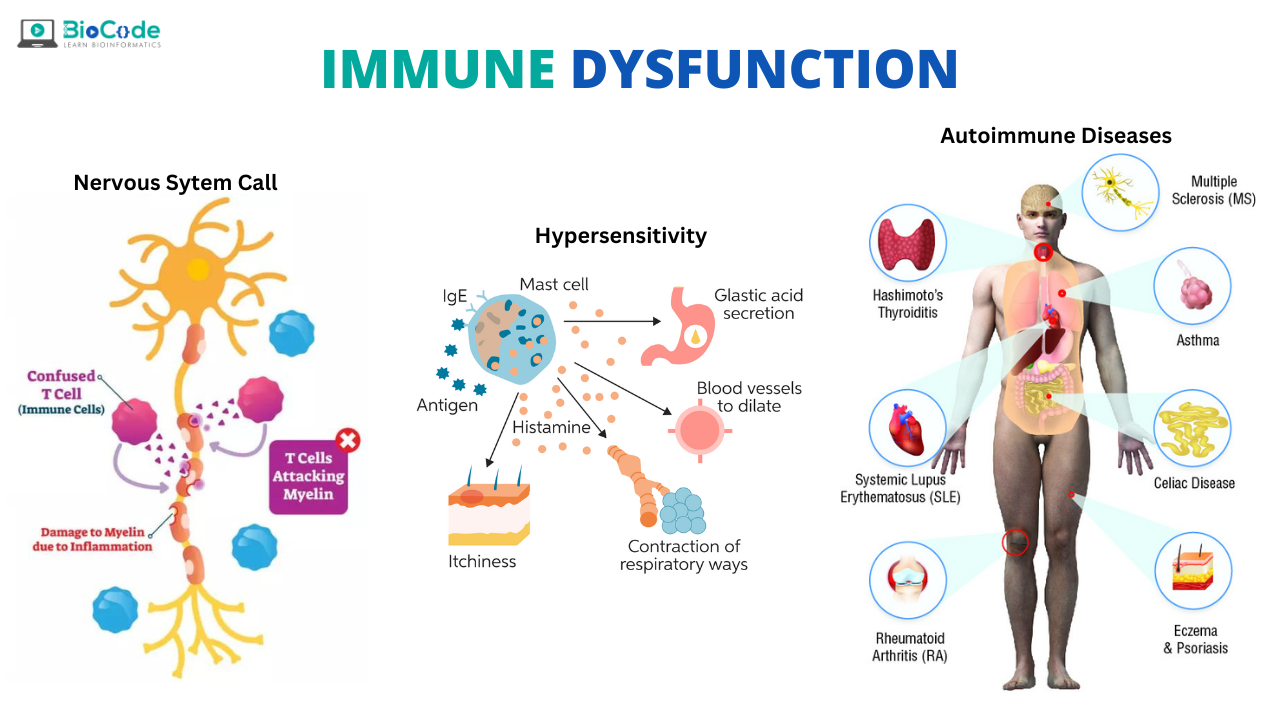
Immune response is a multi-component interactive system that protect host from pathogenic invasion. But failures in the functioning of this system do occur but rarely. These failures can be dramatic and often garner great deal of attention. Immune dysfunction occurs as a result of improper regulation that allows the immune system to either attack something it shouldn’t or fail to attack something it should.
Categories of Immune Dysfunction:
There are three broad categories of immune dysfunction.
Hypersensitivity (including allergy):
The overly zealous attacks on common benign but foreign antigens is hypersensitivity
Autoimmune Disease:
The erroneous targeting of self-proteins or tissues by immune cells leads to autoimmune diseases.
Immune Deficiency:
The insufficiency of the immune response to protect against infectious agents.
Hypersensitivity Reactions
Hypersensitivity results from inappropriate and overly active immune responses to common innocuous environmental antigens, such as pollen, food, or animal dander. The possibility that certain substances induce increased sensitivity (hypersensitivity) rather than protection was recognized in about 1902 by Charles Richet. There are several different types of hypersensitivity reactions; some are caused by antibodies and others are the result of T-cell activity. Most allergic or anaphylactic responses involve a type of antibody called immunoglobulin E (IgE). Binding of IgE to its specific antigen (allergen) induces the release of substances that cause irritation and inflammation, or the accumulation of cells and fluid at the site. When an allergic individual is exposed to an allergen, symptoms may include sneezing, wheezing and difficulty in breathing (asthma); dermatitis or skin eruptions (hives) and, in severe cases, strangulation due to constricted airways.
Autoimmune Diseases:
Immune system malfunctions and a breakdown in self-tolerance occurs. It can be caused by a sudden inability to distinguish between self and non-self or by a misinterpretation of a self-component as dangerous, causing an immune attack on host tissues. This condition is called autoimmunity. The symptoms of autoimmunity differ, depending on which tissues or organs are under attack. Multiple sclerosis is due to an autoimmune attack on a protein in nerve sheaths in the brain and central nervous system that results in neuromuscular dysfunction. Crohn’s disease and rheumatoid arthritis are also examples of autoimmunity. Both genetic and environmental factors are likely involved in the development of most autoimmune diseases.
Immune Deficiency:
When a component of innate or adaptive immunity is absent or defective, the host suffers from some form of immunodeficiency. Some clinical effects can be mild while other are lethal. There are two types of immune deficiencies.
Primary immune deficiencies:
The immune deficiency that arise due to inherited genetic factors.
Secondary immune deficiencies:
A result of disruption/damage by chemical, physical, or biological agents
Primary Immune Deficiency:
A common type of primary immunodeficiency in North America is a selective immunodeficiency in which only one type of antibody, called Immunoglobulin A is lacking. The symptoms may be an increase in certain types of infections, or the deficiency may even go unnoticed. A very rare but much more extreme deficiency, called severe combined immunodeficiency (SCID), affects both B and T cells and it wipes out adaptive immunity. When untreated, SCID frequently results in death from infection at an early age.
Secondary Immune Deficiency:
The most common form of secondary immunodeficiency is Acquired Immune Deficiency Syndrome (AIDS), resulting from infection with Human Immunodeficiency Virus (HIV). HIV hides in the genome of T helper cells, which are critical to guiding the direction of the adaptive immune response. As the immune attack on the virus mounts, more and more of these TH cells are lost. When the disease progresses to AIDS, so many TH cells have been destroyed or otherwise rendered dysfunctional that a gradual collapse of the immune system occurs. Certain antiretroviral treatments can now prolong life with HIV almost indefinitely. There is neither a vaccine nor a cure for this disease.
Cancer And Immune Response:
Cancer, or malignancy, occurs in host cells when they begin to divide out of control. These cells are self in origin, self-tolerance mechanisms can inhibit the development of an immune response. The detection and eradication of cancerous cells is a challenge. Many tumor cells do express unique or developmentally inappropriate proteins, making them potential targets for immune cell recognition and elimination, as well as targets for therapeutic intervention. Genetic instability of these rapidly dividing cells gives them an advantage in evading immune detection and elimination machinery. Both innate and adaptive elements have been shown to be involved in the process of cancer elimination, although adaptive immunity likely plays a more significant role. The immune response to cancer can have both healing and disease-inducing characteristics. It is shown by associations between inflammation and the development of cancer and the degree to which cancerous cells evolve to become more aggressive and invasive under pressure from the immune system. With the cancer studies there is hope that therapies can be designed to boost or maximize the anti-tumor effects of immune cells while dampening their tumor enhancing activities.